Current debates about healthcare cover topics ranging from how to rein in costs to how to make it more personalized. With the emergence of Big Data analytic tools that can rapidly sequence DNA, test hypotheses, discover new relations, uncover fraud, and so forth, the healthcare sector sits on the cusp of a new era. Exactly where the road will lead remains unclear. What is clear, however, is that Big Data analytics hold the potential of making healthcare much more personal. This is particularly true when it comes to developing treatments for disease. Before this can happen, however, there needs to be more secure data sharing.
In an earlier post entitled Big Data and Better Health, I cited an article by Becky Graebe in which she notes that “four distinct big data pools exist in the US health care domain.” Those pools are:
- Pharmaceutical R&D data
- Clinical data
- Activity (claims) and cost data
- Patient behavior and sentiment data
Graebe reports “there is very little overlap in ownership and integration of these pools, though that will be critical in making big strides with big data in health care. [“What is the future of big data in health care?,” SAS Voices, 6 May 2013] Even if data integration occurs slowly, Hellmuth Broda believes that strides will be made in personalized medicines and treatments. [“Personalized Medicine and Big Data,” Pondering Technology, 30 July 2013] He writes:
“While many doomsayers describe the Pharmaceutical industry as one where the golden days are over and where more and more enterprises are bound to be falling off the ‘Patent Cliff’ or get lost in space, many rather visionary companies have ignited their rocket boosters and are catapulting themselves onto firm ground again. This rocket booster consists of treatments for rare diseases and Personalized Medicine. The two chambered booster combines especially targeted diagnostics with targeted therapies and utilises cloud services alongside with Big Data analytics. This new method of transport brings with it new demands on research, clinical trials, production, logistics, information systems and the overall business model.”
To achieve maximum benefit from Big Data analytics, Broda agrees with Graebe that more integration and cooperation needs to occur. He also lists a number of challenges facing the pharmaceutical industry. He continues:
“These challenges and more importantly how Pharma companies tackle them, are shaping the future of the industry, with some key trends already emerging:
- To solve complex tasks, ‘coopetition’ with other companies will become the norm
- The journey towards Personalized Medicine
- Race to Biologics
- Pairing of drugs with their accompanying diagnostics
- Stricter regulations on compliance
- New demands on privacy and security
- Big Data approaches yielding new insight into drug action correlations
“These challenges put new demands on governance, processes, business models and the information systems, which will build the foundation for these new endeavours. New trends in technology adaptation will support and enable these objectives.”
The ability to gather and analyze Big Data is the common thread that weaves it way through all of the trends identified by Broda. One of the dilemmas that will confront the healthcare sector regarding personalized medicines will be cost. Broda explains:
“Drugs will become less generic (and low-cost) and more tailored for specific demographics in the future (and more high value/high cost). There are huge benefits to this, including the fact that these drugs are harder to copy so they retain their value better for the producer and they are also more effective as they can meet more specialist needs. While the current trend is looking at groups of people, maybe based on age or ethnicity, this will evolve in the 21st Century into truly personalized drugs on an individual basis reflecting the patient’s genetic predisposition.”
There are good reasons why doctors and patients alike would like to see more personalized medicines. As Broda explains, “This increasing personalization of therapy will significantly benefit patients, by both raising efficacy and reducing side-effects.” While drug companies may relish the thought of developing high value/high cost drugs, that’s probably not good news for the masses. If Big Data analytics can be used to bring the cost of drug development down, a win-win situation could develop. It has been proven that profits can still be made by selling products to the so-called “bottom billion” consumers if products can be produced at the right price point in the right amount. Big Data analytics should be able to help pharmaceutical companies with that challenge as well. No one benefits when pharmaceutical companies go out of business or when medicines are manufactured in unsafe conditions in poorly regulated plants. For the immediate future, however, it looks like personalized medicines are going to benefit the rich more than the poor.
Broda makes the point that “drugs and their diagnostics walk hand-in-hand.” As I pointed out in my earlier post (mentioned above), Big Data and cognitive reasoning systems are playing a role in diagnostics as well as drug development. A paper from the Institute of Medicine, entitled Making the Case for Continuous Learning from Routinely Collected Data, asserts that a “a learning health system” will be beneficial in a number of ways.
“The availability and reliability of large volumes of relevant longitudinal digital data from a variety of clinical and nonclinical sources are core features of a system that learns from each care experience, a learning health system. Common clinical repositories include data from electronic health record (EHR) systems used to manage patient care and claims data necessary for billing purposes. In some cases, data sources can be linked, using either institution-specific identifiers or matching algorithms, to create disease-specific patient registries that enable research. Integration of large pools of disparate clinical data from EHRs and claims is a major function of health information exchanges, which will be increasingly important to ensure seamless management of health information across institutions. Nonclinical sources of patient information may also include data from retail sales of over-the-counter medications, dietary supplements, walking and running shoes, and personal preferences and behaviors.”
Although technology is important in the healthcare sector, professionals in that field can’t afford to concentrate only on technology if things are going to get better. Like other business sectors, the healthcare sector needs to keep technology, people, and processes in balance. Deanna Pogorelc reports that Dr. Kevin Fickenscher, president and CEO of the American Medical Informatics Association, made that point at a conference earlier this year. [“The problem with big data in health? Too much focus on technology instead of people/process,” MedCity News, 7 May 2013] Pogorelc reports that Fickenscher told conference participants, “One of the things that has been a problem in healthcare is that we tend to spend too much time talking about the technology and not enough time talking about the people and the process. So my personal bias is that while technology is important […] if we don’t deal with the people and process, we will not solve these other issues; we won’t have good change management, and we won’t have good implementation, which is where the value gets created from large data.”
One of the newest fields being developed that will make healthcare even more personal is nanomedicine. “Nanomedicine, refers to highly specific medical intervention at the molecular level for curing disease or repairing damaged tissues.” [“Nanomedicine,” Associates Degree in Nursing] The article states, “Though in its infancy, could we be looking at the future of medicine? Early clinical trials certainly look promising.” The article was accompanied by the following infographic.
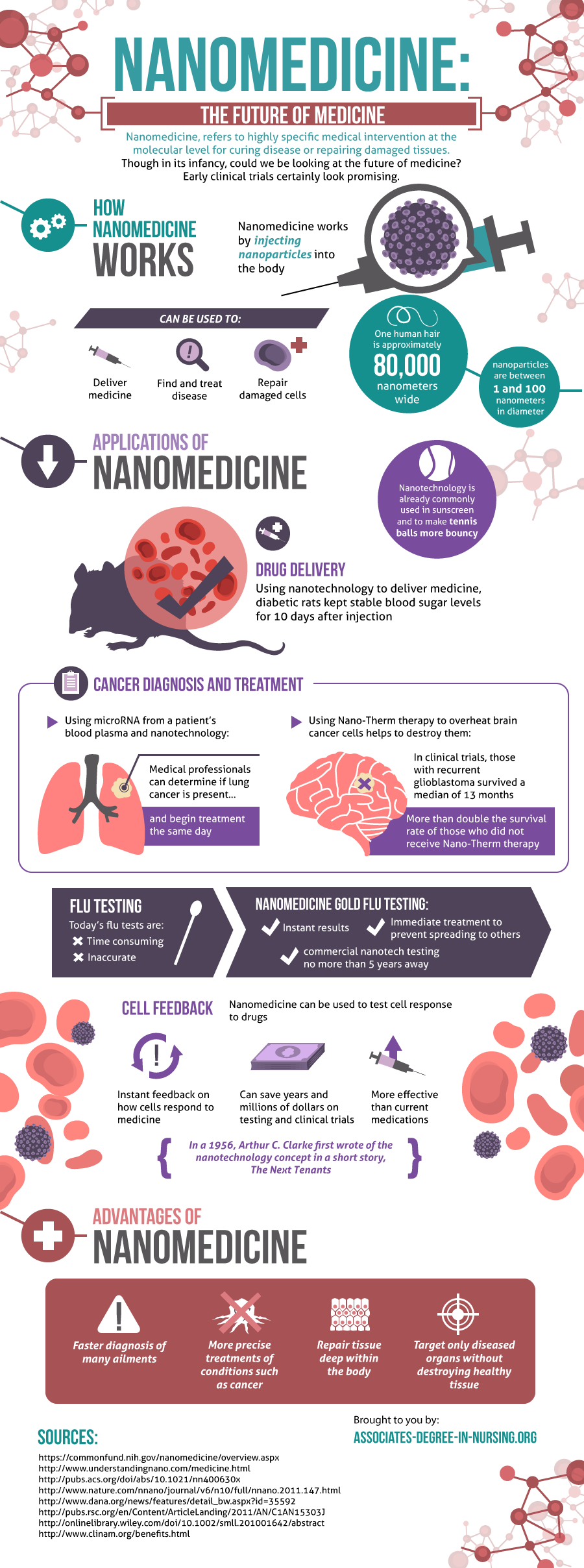
Source: Nanomedicine: The Future of Medicine
It should be abundantly clear that both diagnoses and treatments for diseases are going to be more personal in the future. That should be a good thing; especially if costs can be held in check.




