When Mary Shelly published her novel about Frankenstein’s monster in the early 19th century, she hoped it would serve as a warning about the dangers involved in mankind’s technological evolution during the Industrial Revolution. Her caution, spoken by Dr. Victor Frankenstein, creator of the monster, was, “You seek for knowledge and wisdom, as I once did; and I ardently hope that the gratification of your wishes may not be a serpent to sting you, as mine has been.” Although some fears remain that mad scientists will play God and unleash a crisis upon mankind, the past 200 years have witnessed much more good than evil emerge from laboratories and workshops. I thought it might be interesting to review some of the breakthroughs that have been made recently — at least the ones that have come to my attention. Let’s start at the top and work our way down the body.
The Brain
Samantha Gross reports, “Mind reading may no longer be the domain of psychics and fortune tellers — now some computers can do it, too” [“‘Mind-reading’ brain-scan software showcased in NY,” The Daily Caller, 8 April 2010]. She explains:
“Software that uses brain scans to determine what items people are thinking about [is] among the technological innovations … still under development. The software [by Intel] analyzes functional MRI scans to determine what parts of a person’s brain is being activated as he or she thinks. In tests, it guessed with 90 percent accuracy which of two words a person was thinking about, said Intel Labs researcher Dean Pomerleau. Eventually, the technology could help the severely physically disabled to communicate. And Pomerleau sees it as an early step toward one day being able to control technology with our minds. ‘The vision is being able to interface to information, to your devices and to other people without having an intermediary device,’ he said. For now, the project’s accomplishments are far more modest — it can only be used with prohibitively expensive and bulky fMRI equipment and hasn’t yet been adapted to analyze abstract thoughts.”
Researchers at the University of Maryland are also working on a system that will allow the mind to control technology [“Maryland researchers offer hope of non-invasive portable brain-computer interface,” by Paul Ridden, Gizmag, 7 March 2010]. Ridden reports:
“A study at the University of Maryland has the potential to help movement-impaired people to control the operation of artificial limbs or computer systems without having to undergo extensive training or invasive surgery. The researchers have successfully reconstructed 3D hand movements by decoding electrical brain signals picked up from sensors placed on the scalps of volunteers. The University of Maryland researchers decoded brain signals from five volunteers asked to perform a series of random hand movements while hooked up to an electroencephalography (EEG) machine via 34 sensors around their scalps. The recorded electrical activity data was then translated and reconstructed into 3D hand movements by the team. The researchers discovered that the sensor placed over the primary sensorimotor cortex (which is linked to voluntary movement) appeared to offer more accurate information than the others. More useful data came from the sensor located above the inferior parietal lobule, an area associated with guiding limb movement. … It is believed that the non-invasive, portable technique could be of use to those with severe disabilities and allow them to operate such things as a motorized wheelchair, a prosthetic limb or a robotic device using only a headset containing scalp sensors and the power of thought. The findings may also result in improvements to existing EEG-based systems which facilitate computer interaction by translating brain activity so that current extensive training regimes can be reduced.”
While those breakthroughs could make life much easier for individuals with mobility impairments, other research is going on in areas that will help people with failing memories [“A Little Black Box to Jog Failing Memory,” by Yudhjit Bhattacharjee, New York Times, 8 March 2010]. Bhattacharjee reports on a concept to help people with Alzheimer’s Disease hold on to their memories.
“The concept [is] simple: using digital pictures and audio to archive an experience like a weekend visit from the grandchildren, creating a summary of the resulting content by picking crucial images, and reviewing them periodically to awaken and strengthen the memory of the event. The hardware is a little black box called the SenseCam, which contains a digital camera and an accelerometer to measure movement. Worn like a pendant around the neck, it was developed at Microsoft’s research lab in Cambridge, England. Vicon, a British company that has licensed the technology, is selling its version of the SenseCam only to researchers. For the elderly, though, it could herald a new kind of relationship between mind and machine: even as plaque gets deposited on the brain, everyday experience is deposited on silicon, then retrieved. Researchers say the technology could benefit not just patients but also family and friends, helping them avoid the routine of repeating conversations over and over.”
The Eye
For those old enough to remember the television series “The Bionic Man,” you might recall that it was about a former astronaut who had a serious accident that left him crippled. The opening catch-phrase of the show was “We can rebuild him — we have the technology.” Researchers in Australia are, in fact, trying to build a bionic eye [“First advanced prototype revealed for the Australian bionic eye,” by Loz Blain, Gizmag, 31 March 2010]. Blain reports:
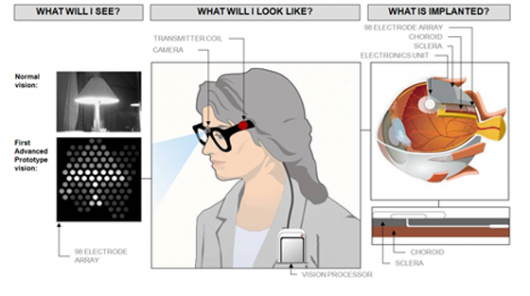 “Researchers at Bionic Vision Australia (BVA) have produced a prototype version of a bionic eye implant that could be ready to start restoring rudimentary vision to blind people as soon as 2013. The system consists of a pair of glasses with a camera built in, a processor that fits in your pocket, and an ocular implant that sits against the retina at the back of the eye and electronically stimulates the retinal neurons that send visual information to the brain. The resulting visual picture is blocky and low-res at this point, but the technology is bound to improve, and even in its current form it’s going to be a major life-changer for those with no vision at all. And the future potential – even for sighted people – is fascinating. … The challenge in bionic eye design is not to get a signal through to the brain, but to improve the resolution and detail of that signal. The first version of the Argus system had only 16 electrodes, so it effectively sent a 16-‘pixel’ image to the brain. The next-gen Argus II carries 60 electrodes. The prototype unveiled this week by BVA is a little more advanced, but still quite rudimentary in the scheme of things. It offers 100 electrodes – so the eventual picture will still be blocky and difficult for somebody with normal vision to interpret. … The second prototype model they’re working on for its first trial run in 2013 is more exciting – with 1000-electrode resolution, the picture will become a lot clearer for patients who receive the implant. We’re talking 20/80 vision, or more than enough to recognize faces, read large print and generally integrate much better into a visually-focused world.”
“Researchers at Bionic Vision Australia (BVA) have produced a prototype version of a bionic eye implant that could be ready to start restoring rudimentary vision to blind people as soon as 2013. The system consists of a pair of glasses with a camera built in, a processor that fits in your pocket, and an ocular implant that sits against the retina at the back of the eye and electronically stimulates the retinal neurons that send visual information to the brain. The resulting visual picture is blocky and low-res at this point, but the technology is bound to improve, and even in its current form it’s going to be a major life-changer for those with no vision at all. And the future potential – even for sighted people – is fascinating. … The challenge in bionic eye design is not to get a signal through to the brain, but to improve the resolution and detail of that signal. The first version of the Argus system had only 16 electrodes, so it effectively sent a 16-‘pixel’ image to the brain. The next-gen Argus II carries 60 electrodes. The prototype unveiled this week by BVA is a little more advanced, but still quite rudimentary in the scheme of things. It offers 100 electrodes – so the eventual picture will still be blocky and difficult for somebody with normal vision to interpret. … The second prototype model they’re working on for its first trial run in 2013 is more exciting – with 1000-electrode resolution, the picture will become a lot clearer for patients who receive the implant. We’re talking 20/80 vision, or more than enough to recognize faces, read large print and generally integrate much better into a visually-focused world.”
Seeing through an implant in your eye makes sense, but what about seeing with your tongue? A prototype system that does just that is also under development [“Seeing Tongue, Spray-On Skin, Transplanted Hand: Top Officer Encounters Military’s Extreme Medicine Wing,” by Noah Shachtman, Wired, 19 April 2010]. Shachtman reports:
“White-haired Clarence ‘Butch’ Schultz, who last served in the Navy in the 1950s, … [has] lost sight in both of his eyes. But a device under investigation [at the University of Pittsburgh Medical Center] has enabled his brain to route around his damaged eyes. The Brainport uses a digital video camera, housed on a pair of sunglasses, to collect visual data. The data is transmitted to a handheld unit, which converts the data to electrical impulses. Those impulses are then sent to an electrode array that’s placed on the tongue (saliva is a great electrical conductor, and the tongue offers densely packed nerves to collect and transmit the impulses to the brain). The device then converts the data to pixels — and allows Schulz to experience the world. ‘I can actually see the difference between light and dark, between cement and black top, between the lawn and the driveway,’ Schultz said. With [Chairman of the Joint Chiefs of Staff Admiral Michael] Mullen and his wife and staff watching, Schultz put down his cane. He shuffled down a laboratory hallway, side-stepping a swivel-chair and a small garbage pail. He’s planning a much longer walk this summer: a 1000-mile trip to his home in Florida.”
As during other periods of conflict, the military is faced with trying to help heal thousands of wounded military personnel. The research being conducted at the University of Pittsburgh Medical Center is at the cutting edge of what can be done. Shachtman calls this “bleeding-edge research into the science of rebuilding human muscle, tissue, and minds.” One researcher, Dr. Douglas Kondziolka, told Admiral Mullen it could take “another decade before his treatment of transplanted brain cells might be widely available to troops who have suffered in war.”
The Skin
Another research project underway at University of Pittsburgh Medical Center is spray-on skin. Shachter reports:
“[During Admiral Mullen’s visit,] Dr. Alain Corcos took a silver rod, tipped with a glowing blue light. He pointed the rod at an easel of white paper, and squirted it with a fine blue mist. When the spray gun is loaded with a compressed air and solution of stem cells and epidermal progenitor cells, it can be used to assist the badly burned. The cells start to divide, eventually covering and healing an area far greater that a traditional skin graft. On one patient, a patch of spray-on skin the size of a postage stamp grew to repair an entire arm. The military has identified 40 troops for future trials, and 40 more civilians have been picked, as well.”
The Medical Center at the University of Pittsburgh isn’t the only lab making advancements in skin research. “Scientists at Spain’s University of Granada have created artificial skin with the resistance, firmness and elasticity of real skin” [“Scientists create artificial skin that stretches like the real thing,” by Ben Coxworth, Gizmag, 28 April 2010]. Coxworth reports:
“It is the first time artificial skin has been created from fibrin-agarose biomaterial. Fibrin is a protein involved in the clotting of the blood, while agarose is a sugar obtained from seaweed, commonly used to create gels in laboratories. The new material could be used in the treatment of skin problems, and could also replace test animals in dermatological labs. … Previously, artificial skin has been made from biomaterials such as collagen, polyglycolic acid, and chitosan. The fibrin-agarose skin, however, looks particularly promising.”
Limbs
Lost limbs are one the challenges created by conflict no matter where it occurs in the world. Although Shachter reports that doctors successfully transplanted a hand from a cadaver to replace one lost by Corporal Josh Maloney, it isn’t a procedure that holds a lot of promise for the majority of people who have lost limbs around the world. A lot of work, however, is being done with artificial limbs. For example, a new foot is being developed that literally puts the spring back in the step of amputees [“Energy recycling artificial foot is a step in the right direction for amputees,” by Darren Quick, Gizmag, 17 February 2010]. Quick reports:
“Most of us take it for granted, but walking isn’t as simple as it looks. With the natural human gait the ankle exerts force to push off the ground. A typical prosthesis doesn’t reproduce the force exerted by a living ankle, resulting in amputees spending much more energy in comparison to walking naturally. A new prototype
artificial foot recycles energy that is otherwise wasted in between steps to significantly cut the energy spent per step, making it easier for amputees to walk. The prosthetic foot created by Art Kuo, professor in the University of Michigan (U-M) departments of Biomedical Engineering and Mechanical Engineering, and U-M graduate, Steve Collins, was designed to capture the energy that is wasted when the ankle hits the ground. To enhance the power of the ankle push-off a microcontroller tells the foot to return the energy at precisely the right time.”
Melding Man with Machine
Fans of Star Trek are well aware of the Borg (“Resistance is futile!”). The Borg become borg-like as a result of having technology fused with their biological systems. In Star Trek television shows and movies, the Borg are the enemy. In real life, however, the melding of technology with biological systems holds great promise [“Silicon computer chips successfully implanted in living human cells,” by Darren Quick, Gizmag, 28 March 2010]. Quick reports:
“Scientists have begun integrating electronics into biology, but don’t bolt your doors in fear of cyborgs and hybrid human-robots yet! Researchers from the Instituto de Microelectrónica de Barcelona IMB-CNM (CSIC), have found a way to implant minute silicon chips into living cells and use them as intracellular sensors. This bio-nanotechnological advancement could tell us a lot about how our cells are working at a nano level, and have widespread implications for early detection of diseases, and new cellular repair mechanisms. … CMOS or Complementary Metal–Oxide–Semiconductor is a technology for constructing integrated circuits, also known as IC, microcircuit, microchip, silicon chip, or chips. These are miniaturized electronic circuits that have been manufactured in the surface of a thin substrate of semiconductor material, and are used in almost all electronic equipment today. A typical human cell is the size of about 10 square micrometers and with transistors the size of nanometers, hundreds of today’s smallest transistors could fit inside a single cell. It was therefore only a matter of time before scientists began interfacing nanoelectronic components with living cells. … The main applications of future intracellular chips will be the study of individual cells. The technology could significantly aid early detection of diseases and new cellular repair mechanisms.”
In an article published a week later, Quick reports on another type of implantable device [“New tissue-hugging implants using flexible electronics,” Gizmag, 28 March 2010]. He reports:
“In what represents the first use of [flexible silicon] for a medical application a team of cardiologists, materials scientists, and bioengineers has created and tested a new type of implantable device for measuring the heart’s electrical output that the team says is a vast improvement over current devices and could also mark the beginning of a new wave of surgical electronics. … New technology that is the result of a collaboration between researchers at Northwestern University and the Universities of Illinois at Urbana-Champaign and Pennsylvania allows the full power of silicon electronics to be directly applied to body tissue. Consisting of a flexible sensor array that can wrap around the heart to map large areas of tissue at once, the new device allows for measuring electrical activity with greater resolution in time and space. The new device can also operate when immersed in the body’s salty fluids and can collect large amounts of data from the body at high speed. … By bringing electronic circuits right to the tissue, rather than having them located remotely, the device can process signals right at the source. This close contact allows the device to have a much higher number of electrodes for sensing or stimulation than is currently possible in medical devices. The researchers say the new device will be able to map the body’s complicated electrical networks in much more detail, with more effective implantable medical devices and treatments likely to emerge.”
Printing Body Parts
A story in The Economist claims “a machine that prints organs is coming to market” [“Making a bit of me,” 18 February 2010]. The article reports:
“The great hope of transplant surgeons is that they will, one day, be able to order replacement body parts on demand. At the moment, a patient may wait months, sometimes years, for an organ from a suitable donor. During that time his condition may worsen. He may even die. The ability to make organs as they are needed would not only relieve suffering but also save lives. And that possibility may be closer with the arrival of the first commercial 3D bio-printer for manufacturing human tissue and organs. The new machine, which costs around $200,000, has been developed by Organovo, a company in San Diego that specialises in regenerative medicine, and Invetech, an engineering and automation firm in Melbourne, Australia. One of Organovo’s founders, Gabor Forgacs of the University of Missouri, developed the prototype on which the new 3D bio-printer is based. The first production models will soon be delivered to research groups which, like Dr Forgacs’s, are studying ways to produce tissue and organs for repair and replacement. At present much of this work is done by hand or by adapting existing instruments and devices. To start with, only simple tissues, such as skin, muscle and short stretches of blood vessels, will be made, says Keith Murphy, Organovo’s chief executive, and these will be for research purposes. Mr Murphy says, however, that the company expects that within five years, once clinical trials are complete, the printers will produce blood vessels for use as grafts in bypass surgery. With more research it should be possible to produce bigger, more complex body parts. Because the machines have the ability to make branched tubes, the technology could, for example, be used to create the networks of blood vessels needed to sustain larger printed organs, like kidneys, livers and hearts.”
The article states that the “3D bio-printer works in a similar way to some rapid-prototyping machines used in industry to make parts and mechanically functioning models.” To learn more about those machines, read my blog entitled Where is My Replicator? The article continues:
“Researchers have found that … when small clusters of cells are placed next to each other they flow together, fuse and organize themselves. Various techniques are being explored to condition the cells to mature into functioning body parts—for example, ‘exercising’ incipient muscles using small machines.”
The article notes that even though “printing organs is new, growing them from scratch on scaffolds has already been done successfully.” It explains:
“In 2006 Anthony Atala and his colleagues at the Wake Forest Institute for Regenerative Medicine in North Carolina made new bladders for seven patients. These are still working. Dr Atala’s process starts by taking a tiny sample of tissue from the patient’s own bladder (so that the organ that is grown from it will not be rejected by his immune system). From this he extracts precursor cells that can go on to form the muscle on the outside of the bladder and the specialized cells within it. When more of these cells have been cultured in the laboratory, they are painted onto a biodegradable bladder-shaped scaffold which is warmed to body temperature. The cells then mature and multiply. Six to eight weeks later, the bladder is ready to be put into the patient.”
The eventual goal of medical science is to use stem cells so that a person’s body can regrow damaged or missing parts. Reports of “engineered stem cells” brings that day closer than ever before. To read more on that topic see my post entitled MIT Technology Review’s Ten Technologies Predicted to Change the World. As I wrote in that post: “I don’t think that there is much doubt that stem cell therapy holds great promise for the future. People with degenerative diseases and spinal column injuries can’t wait for the day that damaged tissues can be replaced by new, healthy material produced by their own bodies.”
Recent experiments are looking at artificial cell structures and synthetic cells. Some of the artificial cell structure research is being done at MIT and Harvard [“Building artificial organs using ‘biological Legos’,” by Darren Quick, 17 May 2010]. Quick explains:
“Researchers at the MIT-Harvard Division of Health Sciences and Technology (HST) have devised a new way to achieve [growing 3D cell cultures that more closely resemble those inside the human body] by using ‘biological Legos’. Tissue engineering has long held promise for building new organs to replace damaged ones, like livers, or blood vessels and other body parts. However, one major obstacle is getting cells grown in a lab dish to form 3D shapes instead of flat layers. To overcome this problem the researchers have encapsulated living cells in cubes and arranged them into 3D structures, just as a child would construct buildings out of blocks. The new technique, dubbed ‘micromasonry’, employs a gel-like material that acts like concrete, binding the cell ‘bricks’ together as it hardens. The tiny cell bricks hold potential for building artificial tissue.”
More controversial was the recent announcement that scientists had created a new form of life using synthetic cells [“Did Scientists Create a Synthetic Cell? It Depends Who You Ask,” by Jacquelyn K. Beals, PhD, Medscape Today, 24 May 2010]. Beals reports:
“Scientists at the Venter Institute have reported the creation of the first ‘synthetic cell’ — Mycoplasma capricolum cells that received and are controlled by a laboratory-assembled genome of Mycoplasma mycoides. Although some scientists note that only the genome is synthetic, the developers explain that the recipient cell’s cytoplasm is diluted with each division. Thus, after 30 generations in culture, some progeny not only have a chromosome of synthetic origin but also contain no proteins from the original cell. … Jim Collins, PhD, professor, Department of Biomedical Engineering, and codirector of the Center for BioDynamics, College of Engineering, Boston University, Massachusetts, responded to the hype: ‘The work … is an important advance in our ability to re-engineer organisms; it does not represent the making of new life from scratch,’ he pointed out. Dr. Collins considers the ‘synthetic cell’ as synthetic only ‘in the sense that its DNA is synthesized, not in that a new life form has been created. Its genome is a stitched-together copy of the DNA of an organism that exists in nature, with a few small tweaks thrown in. … Frankly,’ said Dr. Collins, ‘scientists do not know enough about biology to create life.'”
All of these breakthroughs are promising. Unfortunately, many of them will likely be expensive to implement in the near-term. True medical breakthroughs are those with the potential to help billions of people, not simply the wealthy. Nevertheless, it is essential that researchers continue to test the limits of science. In 1929, John Dewey wrote, “Every great advance in science has issued from a new audacity of imagination.” Although medical science is likely to bump against ethical concerns (such as the cloning of human beings), researchers need to be motivated by a certain audacity of imagination in order to further the frontiers of the medicine.




